You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Euthanasia
- Thread starter Gary
- Start date
Palinurus
The Living Force
Recent new data about the situation in Belgium can be found in the New England Journal of Medicine:
Correspondence
Recent Trends in Euthanasia and Other End-of-Life Practices in Belgium
N Engl J Med 2015; 372:1179-1181 March 19, 2015 DOI: 10.1056/NEJMc1414527
<snip>
The rate of euthanasia increased significantly between 2007 and 2013, from 1.9 to 4.6% of deaths. The overall increase relates to increases in both the number of requests (from 3.5 to 6.0% of deaths) and the proportion of requests granted (from 56.3 to 76.8% of requests made).
After a decrease from 3.2% in 1998 to 1.8% in 2007, the rate of hastening death without an explicit request from the patient remained stable at 1.7% in 2013.
After an increase from 8.2% in 2001 to 14.5% in 2007, the rate of use of continuous deep sedation until death decreased to 12.0% in 2013.
<snip>
Palinurus
The Living Force
Political turmoil around aid-in-dying legislation in Massachusetts and Connecticut lately:
Source: _http://www.courant.com/politics/hc-aid-in-dying-battle-ct-20150322-story.html#page=1
Catholic Church Poised For Pivotal Role In Aid-In-Dying Bill
By Daniela Altimari March 22 2015 8.44 AM
Polls consistently showed broad support for a 2012 ballot initiative in Massachusetts to permit doctors to prescribe a lethal dose of medicine to terminally ill patients.
Then, just weeks before the vote, Catholic institutions and donors stepped in, spending tens of thousands of dollars on a sophisticated TV ad campaign aimed at persuading voters that "physician-assisted suicide" represents a dangerous devaluation of life that could harm society's most vulnerable.
The question was defeated by a scant 2 percentage points.
The political arm of the Roman Catholic Church in Connecticut is determined to quash the issue in this state, as well.
<snip>
"Massachusetts is a fascinating case study and a template for Connecticut,'' said Peter Wolfgang, executive director of the Family Institute of Connecticut and an outspoken opponent of aid in dying.
"Our opponents think there are people out there, like the big bad Catholic church, who want to keep people alive against their will and want them to suffer,'' Wolfgang said. "What we're really talking about is licensing doctors to prescribe a death cocktail and receive legal immunity for it.''
But supporters of the proposal have homed in on the church's high-profile role. In their view, efforts by Catholic leaders to prevent dying patients from exercising a profoundly intimate choice at the end of life echoes earlier struggles.
"This is the same organization that spent money to fight gay rights, the morning-after pill for rape victims, insurance coverage for contraception, civil unions and same-sex marriage,'' said Betty Gallo, a lobbyist for Compassion & Choices, a national group promoting aid-in-dying legislation in statehouses around the nation.
"Connecticut citizens overwhelmingly supported every one of those rights becoming law and they support aid in dying too. The Catholic Church has been on the wrong side of every social issue of our time and they are on the wrong side of this one, too," said Gallo, a veteran Capitol lobbyist for progressive causes such as gay rights and gun control.
The church is deeply invested in efforts to stop the legislation. It is sponsoring a multimedia public relations campaign that includes print and radio spots, as well as ads on buses. Letters were inserted into church bulletins and some parishes have sponsored forums on the topic. And the Catholic conference has retained two outside lobbying firms — Reynolds Strategy Group and Updike, Kelly and Spellacy — to advocate against the bill.
<snip>
Source: _http://www.courant.com/politics/hc-aid-in-dying-battle-ct-20150322-story.html#page=1
Palinurus
The Living Force
Recent overview of latest issues in the Netherlands:
Source: _http://www.dutchnews.nl/features/2015/07/rise-in-euthanasia-requests-sparks-concern-as-criteria-for-help-widen/
Rise in euthanasia requests sparks concern as criteria for help widen
July 3, 2015
Since 2002, euthanasia has been effectively decriminalized in the Netherlands, as long as certain criteria are met. The Dutch position is considered by many to be the blueprint for other countries struggling with right to die issues. Yet, as Gordon Darroch reports, there are concerns in the Netherlands itself about the rise in the number of cases and pressure on patients.
Ruben van Coevorden clearly remembers the first time a patient asked him to help her die. A woman in her 70s who had survived Auschwitz and outlived her husband, but knew she would not overcome lung cancer. ‘She was quite clear-headed about it: she felt she had had her share of suffering and was finished with life,’ says Van Coevorden, who has a medical practice in Amsterdam’s Buitenveldert district. ‘But this was in the days before euthanasia. So I gave her some sleeping pills, enough for an overdose, and stood by her as she took them.’ It was to avoid dilemmas like Van Coevorden’s that the Netherlands passed its euthanasia law in 2001, becoming the first country in the world where doctors were allowed to help their patients to die. ‘Technically, what I did – helping someone to take their own life – was illegal,’ Van Coevorden admits. ‘And it is still punishable, unless certain specific criteria are met.’
Law
The Termination of Life on Request and Assisted Suicide (Review Procedures) Act which health minister Els Borst steered through parliament, did not legalize euthanasia, but gave doctors protection from prosecution if a patient was suffering unbearably and without prospect of improvement (ondraaglijk en uitzichtsloos). The doctor must be satisfied that all alternative forms of treatment have been exhausted or discounted, and seek a second opinion from an independent professional, known as a SCEN doctor (‘support and consultation in euthanasia’). ‘It places a very heavy responsibility on doctors,’ explains Eric van Wijlick, a policy adviser for KNMG, the Dutch medics’ federation. ‘They don’t do it lightly. As a doctor, you’re trained to heal the sick, not to give someone an injection whereby the patient dies.’ In a survey by KNMG, more than half (57%) of doctors who had arranged euthanasia for a patient scored the emotional strain at eight out of 10 or higher. On top of that is the administrative burden: every assisted death case is investigated by one of five regional review committees, who must rule whether the doctor has acted diligently.
All-clear
If not, the prosecution service opens a case file and decides whether to bring criminal proceedings. ‘Most doctors only feel comfortable when the letter arrives, months later, from the review committee giving them the all-clear,’ says Van Wijlick. The Dutch approach to euthanasia has become a focal point for the right-to-die debate in other countries and is regularly invoked by supporters and critics alike, not always accurately. During the 2012 US presidential campaign, the Republican candidate Rick Santorum dramatically claimed that euthanasia accounted for 10% of deaths in the Netherlands, and that half of these were involuntary – the medically-sanctioned murder of elderly patients in hospital. In fact, euthanasia deaths make up just under 3% of the total and doctors need explicit consent from the patient. A more nuanced objection is that endorsing euthanasia in any form is the start of a process of normalizing medically-assisted dying, which will gradually spread into areas currently deemed taboo. Doctors argue that experience has discredited the ‘slippery slope’ argument: only around eight cases a year out of 5,000 are taken up by the prosecution service, and none has led to a conviction. ‘There is no abuse of the system in the Netherlands,’ says Van Coevorden.
Rise
What is inarguable, however, is that the number of euthanasia procedures carried out has risen considerably in 13 years. Initially the annual total hovered at around 1,900, but since 2006 it has increased by an average of 15% a year. In 2013 the number of euthanasia and assisted suicide cases stood at 4,829, nearly three times the 2002 figure. Altogether around 38% of requests are carried out and 20% refused, while in other cases the patient either changes their mind or dies before euthanasia can be arranged.
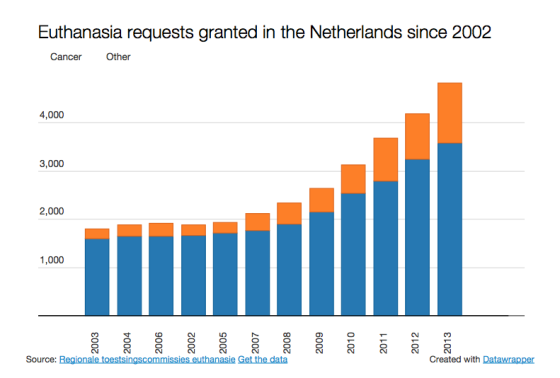
Theo Boer, who spent nine years on one of the regional evaluation committees, sees the rising trend as a cause for concern. Boer, who teaches ethics at the Protestant Theological University in Groningen, argues that the definition of euthanasia in Dutch law is too broad. ‘We don’t have enough specific criteria in the law,’ he says. ‘It doesn’t make any mention of terminal illness, or illness at all. You could have a situation in the Netherlands where somebody goes bankrupt and, knowing he will never get back up to the same level financially, argues he is suffering unbearably and puts in a request for euthanasia.’
Cancer
When the law came in, the overwhelming majority of those who chose euthanasia – nearly 90% – were terminally ill cancer patients. Latterly the proportion has dropped to nearer 75%. The parameters are steadily widening: last month the Dutch paediatrician association NVK called for the minimum age of 12 to be scrapped, arguing that some terminally ill children under that age are capable of deciding they want to die. Psychiatric patients, once never considered for euthanasia, are a small but growing subgroup, with 42 requests granted in 2013. There has been no fall in the suicide rate, as might be expected: in 2013 1,859 Dutch people took their own lives, an unprecedented number. ‘What surprises me is that nobody is making any serious attempt to treat this as a problem,’ says Boer. ‘It seems inarguable to me that the law has led to a rise in incidences. But nobody seems concerned. Even though palliative care has improved considerably, the euthanasia rate has gone up.’
Right to die
Compounding the issue, says Boer, is the fact that euthanasia, which was originally introduced to protect doctors, quickly came to be regarded as a patient’s right. ‘The debate has changed. Euthanasia is no longer a last resort. It was originally seen as a law that gave doctors rights rather than patients. But we very frequently hear it discussed in terms of a patient’s right to euthanasia.’ Boer argues that patients have become more assertive of their preferred way to die. He has been critical of phenomena such as ‘duo-euthanasia’, where the partner of a terminally ill patient asks to die with them because he or she cannot face life alone. ‘When someone has made up their mind they want to die, the first thing they ask is if the doctor can do it,’ he says. And the pressure is not just from patients: ‘In some instances there is pressure from the family.’ Asked to specify a figure from the 4,000 case files that have crossed his desk, Boer replies: ‘It’s hard to say, but at a rough estimate I would say the family is a factor with one in five patients. The doctor doesn’t want to put it in the dossier; you need to read between the lines. Sometimes it’s the family who go to the doctor. Other times it’s the patient saying they don’t want their family to suffer. And you hear anecdotally of families saying: “Mum, there’s always euthanasia”.’
Pressure
The KNMG survey appears to give substance to Boer’s fears on this point: it found that 70% of doctors who replied had felt under pressure to grant euthanasia, while 64% believed the pressure had increased in recent years. The survey did not ask where the pressure came from. Van Wijlick says it is difficult to judge without hard evidence whether there is a problem: ‘We’ve been aware since the early 1990s that pressure is an issue. It would be helpful to do some research into what kind of pressure there is and where it comes from.’ Van Coevorden believes Boer’s figure of one in five is ‘realistic’, adding: ‘I’ve come across it two or three times in my role as a SCEN doctor. There was one case where a woman was dying and had terrible stomach pains, her doctor was tearing his hair out, and when I turned up at the house the family practically pinned me to the wall and said: “You need to give mum the jab now, she’s in agony!” ‘I discovered that her treatment wasn’t working, she was on the wrong type of laxatives and was terribly constipated. I organized a palliative regime that made her more comfortable, and afterwards the family were extremely grateful. She was close to dying anyway, but it allowed them to say goodbye in a better way.’ Van Wijlick argues that the increase in euthanasia deaths shows the system is working. ‘Doctors see from experience that if they follow the procedure, they won’t have difficulties, and they feel reassured. That shouldn’t obscure the fact that doctors find it very hard to carry out. On average they do it once or twice a year and it’s very stressful.’
Aging population
Van Coevorden believes the rise in the number of euthanasia cases is partly due to the aging population. He acknowledges the criteria have widened, but not always in a negative sense, citing the example of a patient in his seventies who had noticed the early signs of dementia. ‘He could have lived several more years, but he’d seen his father decline and didn’t want to go the same way. He had no prospect of relief so he asked me for euthanasia and I agreed. It was clear to me he’d considered it thoroughly.’ What concerns Van Coevorden more is that patients reach for euthanasia too soon. ‘We’ve developed this idea that death can be arranged, but there are other ways to take the pain out of dying, such as palliative sedation, where death occurs naturally. Euthanasia is really the ultimate form of palliative care. But it’s a conflict of duties – the duty to care for a patient versus the duty to prevent their suffering. And it should only be for those exceptional cases.’ He says the Dutch euthanasia law has its roots in the country’s pragmatic instincts. ‘We’re sober-minded and Calvinistic people, we’ve taken the attitude that “this is happening anyway, let’s regulate it”. Dutch doctors don’t have to fear repercussions, they can’t be blackmailed, it’s dealt with openly. We don’t have the kind of situations you get in America.’
Global issue
Van Wijlick agrees: ‘In every country in the world doctors are confronted with the same problem, but there is no way to check if the doctor has acted diligently. We have a transparent system that can accommodate the various different points of view. That’s its strength. The doctor is never obliged to grant euthanasia: the patient has to convince him, and he has to be convinced.’ But Boer strikes a more skeptical note. Though he supports euthanasia in principle and has endorsed thousands of cases, he argues the boundaries should be tighter. ‘If back in the 1990s we had had the quality of palliative care and pain relief that we have now, I doubt whether we would have accepted this euthanasia law at all,’ he says. He regards the law being proposed in Britain by Lord Falconer, which would allow euthanasia only where a patient had a terminal illness, as a better option. ‘We made a number of serious mistakes when we drew up the law,’ says Boer. ‘The problem with being the first country is that you have no precedent. It’s good on some points, such as transparency and evaluation, but in general it’s nothing for us to be proud of. I worry that if death is seen too quickly as the solution, the value of life is reduced.’
Source: _http://www.dutchnews.nl/features/2015/07/rise-in-euthanasia-requests-sparks-concern-as-criteria-for-help-widen/
Palinurus
The Living Force
Recent article on SOTT from The Independent (UK) about machine assisted suicide as a form of legal euthanasia:
http://www.sott.net/article/299410-Australian-right-to-die-doctor-will-gas-audiences-on-television-show-to-model-peaceful-and-reliable-means-of-death
http://www.sott.net/article/299410-Australian-right-to-die-doctor-will-gas-audiences-on-television-show-to-model-peaceful-and-reliable-means-of-death
<snip>
The new Destiny euthanasia machine is said to be much easier to use than its predecessor Deliverance.
Dr Nitschke said the change followed discussions during development in Michigan with Neal Nicol, the assistant of American euthanasia activist Dr Jack Kevorkian, jailed for his direct role in a case of voluntary euthanasia, who died in 2011.
"Suicide is not a crime in the UK, and assistance is not required to use Destiny, which is perfectly legal," Dr Nitschke told The Independent. "The gas that provides the peaceful death is not restricted. Neal Nicol was present at the deaths of over 50 people who died inhaling nine per cent monoxide, and in his opinion, this method is as peaceful and effective as the more difficult administration of intravenous drugs.
"The new Destiny euthanasia machine will provide people with a peaceful and reliable means of death. In Edinburgh I will ask for volunteers and point out that nitrogen only will be used, but as part of the machine display everyone will see the volunteer's cardiac trace projected - the gas can only be switched on if there is a cardiac trace, and switched off as soon as the trace flat-lines."
Deliverance helped four people die in Australia's Northern Territory between 1996-7 in accordance with a state law which came into effect in 1996, but that was overturned a few months later. The machine is now on display in the British Science Museum.
Dr Nitschke said the move to a microprocessor replacing the old laptop means that the new machine is much smaller and also has the ability to be used by people who are seriously disabled, such as quadriplegics, or patients seriously disabled by diseases such as motor neurone disease.
Destiny was initially commissioned after discussion with lawyers for Tony Nicklinson, the 58-year-old right-to-die campaigner who died three years ago having suffered from locked-in syndrome.
His widow Jane continued to fight for a right-to-die ruling but finally lost her case at the European Court of Human Rights last week. She spoke out after the Strasbourg court rejected the case brought by her family and a paralysed former builder, Paul Lamb, saying that the family still believed they would succeed in legalising assisted dying in the UK.
Dr Nitschke said: "What was wanted was a device that could be activated by eye movement, or speech as Tony had, and required minimal assistance to use. I provided the machine details to a recent gathering in San Francisco, including to Neal Nicol, and have now sent them on to two people in the US and New Zealand making enquires for their consideration. There will certainly be more interest when details about Destiny become better known."
<snip>
Thanks for all your updates Palinurus.
This Sott article was posted today, which compliments the 'new Destiny euthanasia machine' article above.
http://www.sott.net/article/299501-Psycho-newspaper-columnist-calls-for-euthanasia-vans-as-Britain-has-far-too-many-old-people
How long before such psychopathic thinking becomes more widespread, as resources diminish (due to environmental disaster/ economic collapse) and a fearful, ignorant populace demand an appropriate response from government authorities. Are these articles on euthansia a form of 'priming' for catastrophic times ahead? I think so. An agenda of eugenics will be invariably (at least initially) window-dressed as 'compassionate' euthansia - with the selfless sacrifice of scared, vulnerable, ill people deemed a 'noble act' for 'the greater good'.
The gentleman I work for 'A', whom I mentioned at the beginning of this thread, suffered a major stroke over 4 months ago now. He is now back in the care home after almost dying in the critical care unit, and then suffering depression as the effects of the stroke became apparent to him - he can no longer swallow, speak, dress or wash himself, nor walk unaided. Yet, he seems very much at peace with himself now, with acceptance of his new life. We still communicate - by hand signals and facial expressions, he still smiles a lot, and we are planning trips out to visit family and friends. I have learned many lessons from this incredibly humbling experience; a few observations are:
* Having spoken to many other stroke victims, the overriding consensus was "I did not appreciate what was truly important in my life, I am grateful for a second chance" and "the signs were there, but I was so stressed, I did not heed them"
* The NHS (National Health Service) is under severe pressure now, the staff who made most difference to 'A' and others, were the ones who could give them the therapy, support and care they desperately needed. The same poorly paid folk who are being pressured by the increasing levels of 'austerity' cuts!
* There are already many people living in the care home who feel they are a burden to their families and society. They feel worthless - primarily because that is how they are made to feel; despite the abundance of knowledge and love they have to share. Such folk have no voice in a sense, so sharing what we can about these issues is a form of speaking on their behalf.
* How would we feel in such circumstances? "There but for the grace of Divine Cosmic Mind go I" as the saying goes. :)
It is also just another reminder of how deeply sick our present society really is - but it is important to keep fighting for truth, compassion and love, to strive to create another 'reality'.
This quote was in the comment box of the aforementioned article and is very apt I feel.
This Sott article was posted today, which compliments the 'new Destiny euthanasia machine' article above.
http://www.sott.net/article/299501-Psycho-newspaper-columnist-calls-for-euthanasia-vans-as-Britain-has-far-too-many-old-people
..."We just have far too many old people," she said. "It's ridiculous to be living in a country where we can put dogs to sleep but not people."
"We need to accept that just because medical advances mean we can live longer, it's not necessarily the right thing to do."
Her solution to the problem? "Easy. Euthanasia vans - just like ice-cream vans - that would come to your home."
"It would all be perfectly charming. They might even have a nice little tune they'd play. I mean this genuinely. I'm super-keen on euthanasia vans," she said...
How long before such psychopathic thinking becomes more widespread, as resources diminish (due to environmental disaster/ economic collapse) and a fearful, ignorant populace demand an appropriate response from government authorities. Are these articles on euthansia a form of 'priming' for catastrophic times ahead? I think so. An agenda of eugenics will be invariably (at least initially) window-dressed as 'compassionate' euthansia - with the selfless sacrifice of scared, vulnerable, ill people deemed a 'noble act' for 'the greater good'.

The gentleman I work for 'A', whom I mentioned at the beginning of this thread, suffered a major stroke over 4 months ago now. He is now back in the care home after almost dying in the critical care unit, and then suffering depression as the effects of the stroke became apparent to him - he can no longer swallow, speak, dress or wash himself, nor walk unaided. Yet, he seems very much at peace with himself now, with acceptance of his new life. We still communicate - by hand signals and facial expressions, he still smiles a lot, and we are planning trips out to visit family and friends. I have learned many lessons from this incredibly humbling experience; a few observations are:
* Having spoken to many other stroke victims, the overriding consensus was "I did not appreciate what was truly important in my life, I am grateful for a second chance" and "the signs were there, but I was so stressed, I did not heed them"
* The NHS (National Health Service) is under severe pressure now, the staff who made most difference to 'A' and others, were the ones who could give them the therapy, support and care they desperately needed. The same poorly paid folk who are being pressured by the increasing levels of 'austerity' cuts!

* There are already many people living in the care home who feel they are a burden to their families and society. They feel worthless - primarily because that is how they are made to feel; despite the abundance of knowledge and love they have to share. Such folk have no voice in a sense, so sharing what we can about these issues is a form of speaking on their behalf.
* How would we feel in such circumstances? "There but for the grace of Divine Cosmic Mind go I" as the saying goes. :)
It is also just another reminder of how deeply sick our present society really is - but it is important to keep fighting for truth, compassion and love, to strive to create another 'reality'.
This quote was in the comment box of the aforementioned article and is very apt I feel.
"Our society must make it right and possible for old people not to fear the young or be deserted by them, for the test of a civilization is the way that it cares for its helpless members."
Pearl Buck, My Several Worlds: A Personal Record (1954)
Palinurus
The Living Force
From: _http://www.news.com.au/lifestyle/health/documentary-makers-expose-horror-for-new-zealand-woman-living-with-cruel-genetic-disorder/story-fneuzlbd-1227478089025
Photos, helpline and video omitted.
Documentary makers expose horror for New Zealand woman living with cruel genetic disorder
August 11, 2015 7:24AM
SHE lives in the dark with a blindfold over her eyes and headphones over her ears.
Sunlight and sound are too much for her fragile body.
A cruel genetic condition makes it impossible for her to use her voice and incredibly painful to move her limbs. She loves hugs but can’t hug back because of the agony it causes.
And her condition will only get worse.
New Zealand woman Gina, whose full name has been withheld, is in her mid 40s. She’s been suffering like this in a dark, silent room for more than a decade. The worst part: doctors don’t know exactly what’s wrong with her.
Gina has told her story for the first time to documentary makers, revealing she has nothing left to live for and just wants to die. The problem is, her government won’t let her.
‘SWAP PLACES WITH ME’
Gina has a simple message for people opposed to voluntary euthanasia: “Swap places with me.”
“I think a compassionate God would want people to have the option of a humane death,” she said.
Wendell Cooke co-directed the documentary Gina with Jeremy Macey. He said he wanted to open people’s eyes to the daily struggle for people living with terminal illnesses.
Speaking with Gina, he said he realised that she and only she should have the right to choose whether or not she goes on living.
“We didn’t go looking for the most extreme case that we could find,” Cooke told news.com.au from his home in Wellington.
“She was living with this atrocious condition. She was disempowered. It’s been really hard and continues to be. Mentally she’s all there, so basically she’s just spending a lot of time thinking.
In the documentary, Gina explains her condition. She uses a touch alphabet to communicate her message.
“I have a rare genetic disorder affected my eyes, ears, larynx and all my joints. I live in enforced darkness and almost silence as sound and light cause further damage to my eyes and ears. My muscles have wasted away. I have total voice loss.”
Cooke said he hoped the documentary would move along a debate that has stagnated in New Zealand following two failed attempts at legalisation.
“We felt that if we could just communicate this to an audience it would go right to the heart of why there needs to be a law change in New Zealand,” he said.
‘I’M NOT A HEARTLESS BASTARD’
Paul Russell is the director of HOPE, an Australian organisation against assisted suicide.
He told news.com.au he feels for Gina but worries that her case could be used to enact damaging legislation.
“It’s obviously difficult for her, she has an incredibly rare condition. I’m not a heartless bastard, I really do feel for these people (but) I can’t see a circumstance where you could enact legislation that would be free from risk for vulnerable people.”
He said the documentary was emotive but “I don’t personalise the issue at all”.
“I’ve got a son with a disability, I’ve been involved in the disability community. I question whether there’s something else that can be done for her (instead of euthanasia).”
Cooke said his film was about not simply “shrugging” and saying “the risks are too great”.
“Objections to legalising voluntary euthanasia seem to centre on the risk of the unknown, risk the that the law could be misused, or risk of the elderly feeling pressured, say by family members, to shorten their lives,” he said.
“These are absolutely valid concerns but my response to that line of argument is it’s not enough to simply shrug and say “the risks are too great” when people are already cruelly suffering under the status quo.
“We should be urging politicians to draft good laws that take these risks into account and manage them for the good of society, the same way we do with other risky endeavours such as driving a car or providing access to alcohol.”
SOME COUNTRIES MOVING, OTHERS STANDING STILL
Australia’s euthanasia laws remain the same as those in New Zealand. But this week the Victorian parliamentary inquiry into end of life choices is hearing from medical professional and palliative care providers about potential changes to Australia’s legislative framework.
Euthanasia is legal in some countries. In Germany and Switzerland it is legal for a doctor to assist in suicide in certain circumstances and in the Netherlands euthanasia was legalised in 2002.
In the US, doctors are allowed to prescribe lethal doses of medicine to terminally ill patients in five US states including Oregon, Vermont and Montana, the Guardian reports.
Gina hopes New Zealand joins that list. Asked how she wanted to die, she told Cooke her doctor would give her medicine and she would fall asleep. Then she would “die peacefully while I hold my sister’s hand”.
Photos, helpline and video omitted.
Palinurus
The Living Force
http://www.sott.net/article/301660-UKs-House-of-Commons-reject-Assisted-Dying-bill
The House of Commons has rejected the Assisted Dying bill by 330 votes to 118, a majority of 212, after an emotional debate Friday afternoon.
The bill proposed giving terminally ill patients the right to request a lethal injection from doctors if their case receive approval from two doctors and a judge.
But the controversial bill, which had been criticized by both the church and campaigners, was voted down on its second reading.
The free vote was the first time the Commons had voted on the issue since 1997.
Throughout the debate, MPs spoke about their personal experiences and used anecdotal evidence to make their case. Many arrived in the chamber saying they were not sure how they would vote.
The bill was based on Oregon law, which opponents said had led to a rise in assisted suicides in the US state since the law was introduced.
continued...
Palinurus
The Living Force
http://www.sott.net/article/301666-Right-to-die-bill-passes-California-Senate-heads-to-Governor
The California State Senate has approved the so-called right-to-die bill following its passage in the State Assembly, despite opposition from religious and disability rights groups. The bill is now awaiting approval from California's Democratic Governor.
The Senate approved the End of Life Option Act in what co-author of the measure Senator Lois Wolk (D-Davis) called a "historic effort." Lawmakers approved the bill on a 23-14 vote after heated debates on Friday, the legislative session's final day.
The Senate has now sent the bill to Governor Jerry Brown. If signed into law, it would allow physicians to prescribe life-ending drugs to terminally ill Californians upon their request.
"Californians want us to act to eliminate the needless pain and prolonged suffering of those who are dying," Wolk told legislators, as cited by the Los Angeles Times.
Wolk predicted earlier that Brown, a lifelong Catholic, would "struggle with this issue" given that the bill has been widely opposed by the Roman Catholic Church and disability rights groups, as well as some doctors and politicians.
"Let's call this what it is. It's not death with dignity. It's assisted killing," said one of the opponents, Republican Senator Robert Huff of San Dimas, as quoted by the Times.
The bill's detractors insist that the legislation requires more work, as there are too many unanswered questions when it comes, for example, to preventing relatives from forcing patients to end their lives prematurely. There have also been concerns that the measure could pose dangers to vulnerable people and those with disabilities, as it could prompt premature suicides.
continued...
Palinurus
The Living Force
Source: _http://www.buzzfeed.com/adolfoflores/california-becomes-fifth-state-to-legalize-doctor-assisted-s#.dggAM98OM
California Becomes Fifth State To Legalize Doctor-Assisted Suicide
Originally posted on Oct. 5, 2015, at 10:28 p.m. Updated on Oct. 6, 2015, at 2:58 a.m.
Adolfo Flores BuzzFeed News Reporter
California became the fifth state in the union to legalize physician-assisted suicide for terminally ill patients on Monday.
In signing the bill, Gov. Jerry Brown said in a statement that he was “left to reflect on what I would want in the face of my own death.”
“I do not know what I would do if I were dying in prolonged and excruciating pain,” Brown said. “I am certain, however, that it would be a comfort to be able to consider the options afforded by this bill. And I won’t deny that right to others.”
The bill — approved by California’s legislature in September — allows doctors to prescribe lethal medication to patients suffering from a terminal illness. The new law is similar to those adopted by Oregon, Washington, and Vermont. A Montana Supreme Court ruling helps protect doctors from prosecution but no physician-assisted suicide laws have been passed.
California’s law has several requirements. Among them:
- That the patient be physically and mentally able to take the lethal drug themselves.
- That the patient make two oral requests, at least 15 days apart, and submit several written requests to their physician.
- The requests must be signed and dated in the presence of two witnesses, one of whom can’t be a family member.
The bill was controversial in part because it was approved during a special legislative session meant to address funding gaps in Medi-Cal coverage. It had previously stalled during the regular session.
Brown said he weighed the pleas from the family of Brittany Maynard, who moved to Oregon in order to take end her own life last year after being diagnosed with terminal brain cancer. The Governor, a former Jesuit seminary student, also listened to concerns from a Catholic bishop, two of his own doctors, and friends.
“ABx2 15 is not an ordinary bill because it deals with life and death,” Brown said in his statement. “The crux of the matter is whether the State of California should continue to make it a crime for a dying person to end his life, no matter how great his pain or suffering.”
The Catholic church was a vocal opponent of the bill, arguing that assisted suicide or euthanasia was unwise and flawed public policy. The group said it put vulnerable patients, particularly the elderly, at risk, and validates suicide as a response to personal mental health problems.
In a statement, Tim Rosales, spokesman for Californians Against Assisted Suicide, said Monday was a dark day for California and Brown’s legacy.
He also expressed concern that Brown’s decision to sign the bill was based on his personal background, which is very different from that of other Californians who don’t have the same access to healthcare.
“These are the people and families potentially hurt by giving doctors the power to prescribe lethal overdoses to patients,” Rosales said. “At this time, the coalition of organizations opposing assisted suicide is looking at all of its options moving forward.”
Adolfo Flores is a reporter for BuzzFeed News and is based in Los Angeles.
Palinurus
The Living Force
Source: _http://www.dutchnews.nl/news/archives/2015/10/euthanasia-death-total-rises-10-in-2014/
Euthanasia death total rises 10% in 2014
October 7, 2015
There was a 10% rise in the number of euthanasia cases in the Netherlands last year, taking the total to 5,306 according to the regional euthanasia monitoring board. The number of cases has risen by around 10% a year for some time. As in previous years, in almost three in four cases the patient had terminal cancer. A spokesman for the monitoring board told the paper [NRC] the increase in euthanasia cases may be related to growing social acceptance of euthanasia.
However, there is likely to be a sharp rise this year in the number of people being helped to die because they had severe psychiatric problems, the NRC says in its report. There were 41 such cases last year, but there are indications this could double in 2015 the NRC says, referring to figures from a special euthanasia clinic published in July. In the first six months of this year, 18 people with severe psychiatric problems were helped to die by the clinic, which was set up in 2012 to help people whose doctors are unwilling to grant euthanasia requests. This is more than double the 2014 total of 17.
Palinurus
The Living Force
Source: _http://www.dutchnews.nl/news/archives/2015/11/voluntary-euthanasia-society-renews-calls-for-end-of-life-pill/
Voluntary euthanasia society renews calls for end-of-life pill
November 13, 2015
The Dutch voluntary euthanasia society [NVVE] is relaunching its campaign to have a pill made available to elderly people who wish to end their lives, the NRC [newspaper] said on Friday. The idea for such a pill was first launched at the beginning of the 1990s by senior judge and euthanasia campaigner Huib Drion and became known as ‘Drion’s pill’. He said the pill should be issued free of charge to everyone over the age of 70 but his initiative floundered on medical, ethical and legal grounds.
Now the NVVE is having a new attempt and this time says the pills should only be issued by pharmacists or family doctors. ‘This is important to make sure that the drugs cannot be used for suicide, abuse or murder,’ the organisation said. The NVVE now wants to discuss its ideas for an experiment with the health and justice ministries and with the Dutch doctors’ association KNMG. ‘We see that society wants such a pill, particularly among the babyboom generation which is not afraid to speak its mind,’ NVVE director Robert Schurink told the NRC. ‘They want control over the end of their lives.’
At the moment, the NVVE helps people who do not want to live any longer access foreign suppliers who can help them buy the pills to do the job, the paper said.
Euthanasia is not legal in the Netherlands but the legislation has given doctors protection from prosecution if a patient was suffering unbearably and without prospect of improvement. Last year, some 14,000 people in the Netherlands were helped to die, most of whom were suffering from cancer.
Palinurus
The Living Force
Source: _http://www.dutchnews.nl/news/archives/2016/01/doctors-should-have-the-right-to-refuse-euthanasia-requests-knmg/
Similar story: _http://www.nltimes.nl/2016/01/05/doctors-demand-right-to-refuse-euthanasia/
Doctors should have the right to refuse euthanasia requests: KNMG
January 5, 2016
Dutch doctors must retain the right to refuse to help their patients to die, the doctors’ federation KNMG has told the NRC.
While most doctors back euthanasia, or assisted dying, they should never be compelled to cooperate, Rutger Jan van der Gaag is quoted as saying. Euthanasia should not be something that can be forced on doctors, he said.
The Dutch voluntary euthanasia society [NVVE] last year relaunched its campaign to have a pill made available to elderly people who wish to end their lives.
Ethical grounds
The idea for such a pill was first launched at the beginning of the 1990s by senior judge and euthanasia campaigner Huib Drion and became known as ‘Drion’s pill’. He said the pill should be issued free of charge to everyone over the age of 70 but his initiative floundered on medical, ethical and legal grounds.
Now the NVVE is having a new attempt and this time says the pills should only be issued by pharmacists or family doctors. ‘This is important to make sure the drugs cannot be used for suicide, abuse or murder,’ the organisation said.
Euthanasia is legal in the Netherlands under strict conditions. For example, the patient must be suffering unbearable pain and the doctor must be convinced the patient is making an informed choice. The opinion of a second doctor is also required.
‘The doctor is currently an important safety catch who makes sure that reasonable alternatives [to euthanasia] are not ignored and that the drugs are not misused,’ Van der Gaag told the NRC.
Similar story: _http://www.nltimes.nl/2016/01/05/doctors-demand-right-to-refuse-euthanasia/
Palinurus
The Living Force
Source: _http://www.nltimes.nl/2016/01/07/euthanasia-okd-for-dementia-patients-who-request-it-when-lucid/
Similar story: _http://www.dutchnews.nl/news/archives/2016/01/euthanasia-rules-relaxed-for-people-with-serious-dementia/
Euthanasia ok’d for dementia patients who request it when lucid
Posted on Jan 7, 2016 by Janene Pieters
The Ministries of Public Health and Security and of Justice updated their “guide” on euthanasia to give people suffering from severe dementia the option of euthanasia, even if they are unable to express the wish themselves. This is only possible if the patient wrote a declaration with his wish for euthanasia while he was still clearheaded, broadcaster NOS reports.
The new guide states that patients with severe dementia often do not seem to be suffering unbearably under their dementia, but they do suffer under the physical conditions that go along with it, such as severe anxiety and pain. “In those cases a doctor may give euthanasia, even if a patient can not make it clear in words or gesture. But there has to be a written request for euthanasia, that the patient drew up earlier.”
The guide was updated to take away the uncertainty about the possibilities for euthanasia in dementia patients. According to the guide, doctors have given euthanasia to dementia patients with a previously written request a few times before. But if it is unclear whether such a request still exist at a time that a patient is unable to express himself, chances are that the doctor will not carry out euthanasia.
The guide includes a manual for drafting a euthanasia declaration. Patients are advised to to stay in discussion with their doctors about euthanasia to ensure that such a declaration is in place if they need it.
Earlier this week doctors federation KNMG demanded that doctors always have the ability to deny an euthanasia request. They do not want to be obligated to perform euthanasia whenever a patient requests it.
Similar story: _http://www.dutchnews.nl/news/archives/2016/01/euthanasia-rules-relaxed-for-people-with-serious-dementia/
Trending content
-
-
-
Thread 'Coronavirus Pandemic: Apocalypse Now! Or exaggerated scare story?'
- wanderingthomas
Replies: 30K -
